Iron deficiency anemia: Difference between revisions
imported>Robert Badgett |
mNo edit summary |
||
| (19 intermediate revisions by 4 users not shown) | |||
| Line 1: | Line 1: | ||
{{subpages}} | {{subpages}} | ||
{{TOC|left}} | |||
{{Infobox_Disease | | {{Infobox_Disease | | ||
Name = Iron deficiency anemia | | Name = Iron deficiency anemia | | ||
| Line 15: | Line 15: | ||
MeshID = D018798 | | MeshID = D018798 | | ||
}} | }} | ||
'''Iron deficiency anemia''' is the most common type of [[anemia]], and the most common cause of [[microcytic anemia]]. | |||
Iron deficiency anemia occurs when the dietary intake or absorption of [[iron]] is insufficient, and hemoglobin, which contains iron, cannot be formed. In the [[United States of America]], 20% of all women of childbearing age have iron deficiency anemia, compared with only 2% of adult men. The principal cause of iron deficiency anemia in premenopausal women is blood lost during [[menstruation|menses]]. | |||
Iron deficiency anemia occurs when the dietary intake or absorption of [[iron]] is insufficient, and hemoglobin, which contains iron, cannot be formed. In the [[United States]], 20% of all women of childbearing age have iron deficiency anemia, compared with only 2% of adult men. The principal cause of iron deficiency anemia in premenopausal women is blood lost during [[menstruation|menses]]. | |||
Iron deficiency anemia is the final stage of [[iron deficiency (medicine)|iron deficiency]]. When the body has sufficient iron to meet its needs (functional iron), the remainder is stored for later use in the [[bone marrow]], [[liver]], and [[spleen]]. Iron deficiency ranges from iron depletion, which yields little physiological damage, to iron deficiency anemia, which can affect the function of numerous [[organ system]]s. Iron depletion causes the amount of stored iron to be reduced, but has no effect on the functional iron. However, a person with no stored iron has no reserves to use if the body requires more iron. In essence, the amount of iron absorbed by the body is not adequate for growth and development or to replace the amount lost. | Iron deficiency anemia is the final stage of [[iron deficiency (medicine)|iron deficiency]]. When the body has sufficient iron to meet its needs (functional iron), the remainder is stored for later use in the [[bone marrow]], [[liver]], and [[spleen]]. Iron deficiency ranges from iron depletion, which yields little physiological damage, to iron deficiency anemia, which can affect the function of numerous [[organ system]]s. Iron depletion causes the amount of stored iron to be reduced, but has no effect on the functional iron. However, a person with no stored iron has no reserves to use if the body requires more iron. In essence, the amount of iron absorbed by the body is not adequate for growth and development or to replace the amount lost. | ||
| Line 28: | Line 27: | ||
Iron deficiency anemia is characterized by [[pallor]], [[fatigue (medical)|fatigue]] and [[muscle weakness|weakness]]. Because it tends to develop slowly, adaptation occurs and the disease often goes unrecognized for some time. In severe cases, [[dyspnea]] can occur. Unusual obsessive food cravings, known as [[pica (disorder)|pica]], may develop. | Iron deficiency anemia is characterized by [[pallor]], [[fatigue (medical)|fatigue]] and [[muscle weakness|weakness]]. Because it tends to develop slowly, adaptation occurs and the disease often goes unrecognized for some time. In severe cases, [[dyspnea]] can occur. Unusual obsessive food cravings, known as [[pica (disorder)|pica]], may develop. | ||
Other symptoms include: | |||
* Cognitive dysfunction<ref name="pmid17344500">{{cite journal |author=Murray-Kolb LE, Beard JL |title=Iron treatment normalizes cognitive functioning in young women |journal=Am. J. Clin. Nutr. |volume=85 |issue=3 |pages=778–87 |year=2007 |pmid=17344500 |doi=}}</ref> | |||
=== | One of the first abnormal values to be noted on a CBC will be a high [[red blood cell distribution width]] (RDW), reflecting a varied population of [[erythrocytes|red blood cells]]. A low [[Mean corpuscular volume|MCV]], [[Mean corpuscular hemoglobin|MCH]] or [[Mean corpuscular hemoglobin concentration|MCHC]], and the appearance of the RBCs on visual examination of a [[peripheral blood smear]] will narrow the diagnosis to a ''microcytic anemia''. | ||
{| class="wikitable" border="1" align="right" | |||
|+ Mean corpuscular volume (MCV) for the predicting a ferritin < 15 ng/ml<ref name="pmid2187961">{{cite journal |author=Seward SJ, Safran C, Marton KI, Robinson SH |title=Does the mean corpuscular volume help physicians evaluate hospitalized patients with anemia? |journal=J Gen Intern Med |volume=5 |issue=3 |pages=187–91 |year=1990 |pmid=2187961 |doi= |url= |issn=}}</ref> | |||
|- | |||
! MCV | |||
! Sensitivity | |||
! Specificity | |||
|- | |||
| < 70 fL | |||
| 24% | |||
| 96% | |||
|- | |||
| < 80 fL | |||
| 48% | |||
| 83% | |||
|- | |||
| < 92 fL | |||
| 88% | |||
| 39% | |||
|} | |||
===Evaluation of iron status=== | |||
{{main|Human iron metabolism}} | |||
The serum [[ferritin]] is the best laboratory test for storage of marrow iron.<ref name="pmid9686711">{{cite journal |author=Kis AM, Carnes M |title=Detecting iron deficiency in anemic patients with concomitant medical problems |journal=J Gen Intern Med |volume=13 |issue=7 |pages=455–61 |year=1998 |month=July |pmid=9686711 |pmc=1496985 |doi= |url= |issn=}}</ref><ref>{{cite journal | author = Guyatt G, Patterson C, Ali M, Singer J, Levine M, Turpie I, Meyer R | title = Diagnosis of iron-deficiency anemia in the elderly. | journal = Am J Med | volume = 88 | issue = 3 | pages = 205-9 | year = 1990 | id = PMID 2178409}}</ref><ref>Guyatt GH, Oxman AD, Ali M, Willan A, McIlroy W, Patterson C.Laboratory diagnosis of iron-deficiency anemia: an overview.J Gen Intern Med. 19927:145-53. Review. (Erratum in: J Gen Intern Med 1992;7:423) PMID: 1487761</ref> However, the accuracy of the [[ferritin]] has not been studied since the World Health Organization used a recombinant [[ferritin]] preparation to create a third, traceable International Standard in 1997.<ref name="pmid9299937">{{cite journal| author=Thorpe SJ, Walker D, Arosio P, Heath A, Cook JD, Worwood M| title=International collaborative study to evaluate a recombinant L ferritin preparation as an International Standard. | journal=Clin Chem | year= 1997 | volume= 43 | issue= 9 | pages= 1582-7 | pmid=9299937 | doi= | pmc= | url=http://www.ncbi.nlm.nih.gov/entrez/eutils/elink.fcgi?dbfrom=pubmed&tool=sumsearch.org/cite&retmode=ref&cmd=prlinks&id=9299937 }} </ref> <ref name="pmid20338782">{{cite journal| author=Thorpe SJ| title=The development and role of international biological reference materials in the diagnosis of anaemia. | journal=Biologicals | year= 2010 | volume= 38 | issue= 4 | pages= 449-58 | pmid=20338782 | doi=10.1016/j.biologicals.2010.02.007 | pmc= | url=http://www.ncbi.nlm.nih.gov/entrez/eutils/elink.fcgi?dbfrom=pubmed&tool=sumsearch.org/cite&retmode=ref&cmd=prlinks&id=20338782 }} </ref> | |||
Other tests that have been used are serum [[iron]] level, and serum [[transferrin]] level. While serum iron varies greatly intra-individually also in response to iron intake, the other two parameters mentioned change in an [[acute phase reaction]] (ferritin rises and transferrin false) and thus cannot reliably detect iron deficiency in the presence of inflammation. They also do not measure if the iron is actually available for hematopoiesis. Modern tests that circumvent this problem include [[soluble transferrin receptor]] (sTfr), [[transferrin saturation]] (TfS or TSAT), the hemoglobin content of [[reticulocyte]]s or the percentage of hypochromic cells <ref>{{cite journal | author = Thomas C, Thomas L | title = Biochemical Markers and Hematologic Indices in the Diagnosis of Functional Iron Deficiency | journal = Clin Chem | volume = 48 | issue = 7 | pages = 1066-76 | year = 2002 | id = PMID 12089176}}</ref>. Most of these can today be readily determined on automated laboratory analysis systems. | |||
= | {| class="wikitable" | ||
|+ [[Likelihood ratio]]s for common tests<ref name="pmid1487761">{{cite journal |author=Guyatt GH, Oxman AD, Ali M, Willan A, McIlroy W, Patterson C |title=Laboratory diagnosis of iron-deficiency anemia: an overview |journal=J Gen Intern Med |volume=7 |issue=2 |pages=145–53 |year=1992 |pmid=1487761 |doi= |url= |issn=}}</ref> | |||
|- | |||
! Test | |||
! Cutoff value | |||
! [[Likelihood ratio]] | |||
|- | |||
| MCV | |||
| align="center" | ≥ 90 m<sup>3</sup> | |||
| align="center" | 0.29 | |||
|- | |||
| MCV | |||
| align="center" | ≤ 70 m<sup>3</sup> | |||
| align="center" | 12.47 | |||
|- | |||
| RDW | |||
| align="center" style="color:gray" | ≤ 15% | |||
| align="center" style="color:gray" | 0.61 | |||
|- | |||
| RDW | |||
| align="center" style="color:gray" | ≥ 21% | |||
| align="center" style="color:gray" | 2.72 | |||
|- | |||
| Ferritin | |||
| align="center" | ≥ 100 ng/ml | |||
| align="center" | 0.08 | |||
|- | |||
| Ferritin | |||
| align="center" | < 25 ng/ml | |||
| align="center" | < 8.83 | |||
|- | |||
| Transferrin saturation | |||
| align="center" | ≥ 50% | |||
| align="center" | 0.15 | |||
|- | |||
| Transferrin saturation | |||
| align="center" | ≤ 5% | |||
| align="center" | 10.46 | |||
|- | |||
| colspan="3"| A [[likelihood ratio]] > 10 helps establish a diagnosis while a ratio < 0.1 helps exclude a diagnosis.<ref name="pmid12213147">{{cite journal |author=McGee S |title=Simplifying likelihood ratios |journal=J Gen Intern Med |volume=17 |issue=8 |pages=646–9 |year=2002 |month=August |pmid=12213147 |doi= |url= |issn=}}</ref> | |||
|} | |||
Iron deficiency is difficult to diagnose in alcoholics.<ref name="pmid3747828">{{cite journal |author=Savage D, Lindenbaum J |title=Anemia in alcoholics |journal=Medicine (Baltimore) |volume=65 |issue=5 |pages=322–38 |year=1986 |month=September |pmid=3747828 |doi= |url= |issn=}}</ref> | |||
{| class="wikitable" align="right" | |||
|+ Diagnosing iron deficiency in alcoholics.<ref name="pmid3747828">{{cite journal |author=Savage D, Lindenbaum J |title=Anemia in alcoholics |journal=Medicine (Baltimore) |volume=65 |issue=5 |pages=322–38 |year=1986 |month=September |pmid=3747828 |doi= |url= |issn=}}</ref> | |||
|- | |||
! Finding | |||
! Cutoff value | |||
! Sensitivity | |||
! Specificity | |||
|- | |||
| MCV | |||
| < 80 m<sup>3</sup> | |||
| 25% | |||
| 97% | |||
|- | |||
| Ferritin | |||
| < 20 ng/ml | |||
| 50% | |||
| 100% | |||
|- | |||
| Transferrin saturation | |||
| ≤ 15% | |||
| 56% | |||
| 87% | |||
|- | |||
| Ferritin | |||
| < 20 ng/ml | |||
| 50% | |||
| 100% | |||
|- | |||
| Ferritin | |||
| < 100 ng/ml | |||
| 100% | |||
| 95% | |||
|} | |||
===Evaluation of underlying causes=== | ===Evaluation of underlying causes=== | ||
| Line 57: | Line 138: | ||
==Treatment== | ==Treatment== | ||
If the cause is dietary iron deficiency, [[iron supplements]], usually with [[iron (II) sulfate]] or iron amino acid chelate, can correct the anemia. Chelated iron | Treating iron deficiency, even in the absence of [[anemia]], can benefit patients with [[heart failure]].<ref name="pmid19920054">{{cite journal| author=Anker SD, Comin Colet J, Filippatos G, Willenheimer R, Dickstein K, Drexler H et al.| title=Ferric carboxymaltose in patients with heart failure and iron deficiency. | journal=N Engl J Med | year= 2009 | volume= 361 | issue= 25 | pages= 2436-48 | pmid=19920054 | ||
| url=http://www.ncbi.nlm.nih.gov/entrez/eutils/elink.fcgi?dbfrom=pubmed&tool=clinical.uthscsa.edu/cite&email=badgett@uthscdsa.edu&retmode=ref&cmd=prlinks&id=19920054 | doi=10.1056/NEJMoa0908355 }}</ref> | |||
If the cause is dietary iron deficiency, [[iron supplements]], usually with [[iron (II) sulfate]] or iron amino acid chelate, can correct the anemia. Chelated iron is ten to fifteen times more bioavailable per mg and has none of the side effects of iron sulfate's sulfur content. If malabsorption is present, it may be necessary to administer iron [[parenteral|parenterally]] (e.g., as [[iron dextran]], which has largely been replaced by [[iron sucrose]]), as on the World Health Organization list of essential medicines, <ref name=WHO>{{citation | |||
| url = http://www.who.int/medicines/areas/quality_safety/safety_efficacy/Addendum.pdf | |||
| publisher = [[World Health Organization]] | |||
| title = The Safety and Iron Dextran and a comparison wit Iron Sucrose for Intravenous Use: a Short Report to the World Health Organization Advisory Committee on the Safety of Medicines | |||
| author = Peter I Folb | |||
| date = 18 October 2004}}</ref> Parenteral iron other than in chelated form, however, is generally poorly tolerated, and the earlier forms of chelated iron, such as iron dextran, were not without risk. The still-available dextran preparation carries a significant risk of [[anaphylactic shock]],<ref name=FDA>{{citation | |||
| url = http://www.fda.gov/Safety/MedWatch/SafetyInformation/SafetyAlertsforHumanMedicalProducts/ucm186899.htm | |||
| title = Dexferrum (iron dextran injection) - Labeling Change | |||
| date = 16 October 2009 | |||
| publisher = [[Food and Drug Administration]]}}</ref> and iron dextran, as opposed to [[iron sucrose]], provided ferrous as well as the desired ferric iron ions. | |||
The replacement dose of iron may be low. | |||
* In the elderly, may be as little as 15 mg per day of elemental iron <ref name="pmid16194646">{{cite journal |author=Rimon E, Kagansky N, Kagansky M, Mechnick L, Mashiah T, Namir M, Levy S |title=Are we giving too much iron? Low-dose iron therapy is effective in octogenarians |journal=Am J Med |volume=118 |issue=10 |pages=1142-7 |year=2005 |id=PMID 16194646 | doi = 10.1016/j.amjmed.2005.01.065}}</ref>. | |||
* In patients with inflammatory bowel disease, 106 mg/day may be adequate in most patients.<ref name="pmid19408339">{{cite journal| author=Gisbert JP, Bermejo F, Pajares R, Pérez-Calle JL, Rodríguez M, Algaba A et al.| title=Oral and intravenous iron treatment in inflammatory bowel disease: hematological response and quality of life improvement. | journal=Inflamm Bowel Dis | year= 2009 | volume= 15 | issue= 10 | pages= 1485-91 | pmid=19408339 | doi=10.1002/ibd.20925 | pmc= | url= }} </ref> | |||
Follow up evaluation with retesting of the [[hemoglobin]] (Hgb), [[hematocrit]] (Hct), and [[erythrocyte indices#mean corpuscular volume|mean corpuscular volume (MCV)]] may help demonstrate whether the treatment has been effective. Testing of the [[reticulocyte]] count is another way to measure a response to iron therapy. Finally, ongoing testing of iron indices via the [[ferritin]] level and maybe [[total iron binding capacity]] (TIBC), and [[serum iron]] levels are imperative to avoid iron overloading. | |||
Iron supplements must be kept out of the reach of children, as iron-containing supplements are a frequent cause of poisoning in the pediatric age group. | |||
"Iron supplementation should be considered for women with unexplained fatigue who have [[ferritin]] levels below 50 μg/L". <ref name="pmid22777991">{{cite journal| author=Vaucher P, Druais PL, Waldvogel S, Favrat B| title=Effect of iron supplementation on fatigue in nonanemic menstruating women with low ferritin: a randomized controlled trial. | journal=CMAJ | year= 2012 | volume= 184 | issue= 11 | pages= 1247-54 | pmid=22777991 | doi=10.1503/cmaj.110950 | pmc=PMC3414597 | url=http://www.ncbi.nlm.nih.gov/entrez/eutils/elink.fcgi?dbfrom=pubmed&tool=sumsearch.org/cite&retmode=ref&cmd=prlinks&id=22777991 }} </ref> In this trial, the average [[mean corpuscular volume]] was normal. | |||
==References== | ==References== | ||
{{reflist}} | |||
==See Also== | ==See Also== | ||
* [[Human iron metabolism]] | * [[Human iron metabolism]] | ||
==External links== | ==External links==[[Category:Suggestion Bot Tag]] | ||
Latest revision as of 06:00, 3 September 2024
| Iron deficiency anemia | |
|---|---|
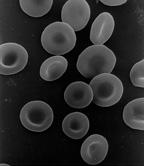
| Red blood cells | |
| ICD-10 | ICD10 F84.0-F84.1 |
| ICD-9 | 280 |
| MeSH | D018798 |
Iron deficiency anemia is the most common type of anemia, and the most common cause of microcytic anemia.
Iron deficiency anemia occurs when the dietary intake or absorption of iron is insufficient, and hemoglobin, which contains iron, cannot be formed. In the United States of America, 20% of all women of childbearing age have iron deficiency anemia, compared with only 2% of adult men. The principal cause of iron deficiency anemia in premenopausal women is blood lost during menses.
Iron deficiency anemia is the final stage of iron deficiency. When the body has sufficient iron to meet its needs (functional iron), the remainder is stored for later use in the bone marrow, liver, and spleen. Iron deficiency ranges from iron depletion, which yields little physiological damage, to iron deficiency anemia, which can affect the function of numerous organ systems. Iron depletion causes the amount of stored iron to be reduced, but has no effect on the functional iron. However, a person with no stored iron has no reserves to use if the body requires more iron. In essence, the amount of iron absorbed by the body is not adequate for growth and development or to replace the amount lost.
History
A disease believed to be iron deficiency anemia is described in about 1500 B.C. in the Egyptian Ebers papyrus. It was termed chlorosis or green sickness in Medieval Europe, and iron salts were used for treatment in France by the mid-17th century. Thomas Sydenham recommended iron salts as treatment for chlorosis, but treatment with iron was controversial until the 20th century, when its mechanism of action was more fully elucidated.
Symptoms
Iron deficiency anemia is characterized by pallor, fatigue and weakness. Because it tends to develop slowly, adaptation occurs and the disease often goes unrecognized for some time. In severe cases, dyspnea can occur. Unusual obsessive food cravings, known as pica, may develop.
Other symptoms include:
- Cognitive dysfunction[1]
One of the first abnormal values to be noted on a CBC will be a high red blood cell distribution width (RDW), reflecting a varied population of red blood cells. A low MCV, MCH or MCHC, and the appearance of the RBCs on visual examination of a peripheral blood smear will narrow the diagnosis to a microcytic anemia.
| MCV | Sensitivity | Specificity |
|---|---|---|
| < 70 fL | 24% | 96% |
| < 80 fL | 48% | 83% |
| < 92 fL | 88% | 39% |
Evaluation of iron status
The serum ferritin is the best laboratory test for storage of marrow iron.[3][4][5] However, the accuracy of the ferritin has not been studied since the World Health Organization used a recombinant ferritin preparation to create a third, traceable International Standard in 1997.[6] [7]
Other tests that have been used are serum iron level, and serum transferrin level. While serum iron varies greatly intra-individually also in response to iron intake, the other two parameters mentioned change in an acute phase reaction (ferritin rises and transferrin false) and thus cannot reliably detect iron deficiency in the presence of inflammation. They also do not measure if the iron is actually available for hematopoiesis. Modern tests that circumvent this problem include soluble transferrin receptor (sTfr), transferrin saturation (TfS or TSAT), the hemoglobin content of reticulocytes or the percentage of hypochromic cells [8]. Most of these can today be readily determined on automated laboratory analysis systems.
| Test | Cutoff value | Likelihood ratio |
|---|---|---|
| MCV | ≥ 90 m3 | 0.29 |
| MCV | ≤ 70 m3 | 12.47 |
| RDW | ≤ 15% | 0.61 |
| RDW | ≥ 21% | 2.72 |
| Ferritin | ≥ 100 ng/ml | 0.08 |
| Ferritin | < 25 ng/ml | < 8.83 |
| Transferrin saturation | ≥ 50% | 0.15 |
| Transferrin saturation | ≤ 5% | 10.46 |
| A likelihood ratio > 10 helps establish a diagnosis while a ratio < 0.1 helps exclude a diagnosis.[10] | ||
Iron deficiency is difficult to diagnose in alcoholics.[11]
| Finding | Cutoff value | Sensitivity | Specificity |
|---|---|---|---|
| MCV | < 80 m3 | 25% | 97% |
| Ferritin | < 20 ng/ml | 50% | 100% |
| Transferrin saturation | ≤ 15% | 56% | 87% |
| Ferritin | < 20 ng/ml | 50% | 100% |
| Ferritin | < 100 ng/ml | 100% | 95% |
Evaluation of underlying causes
The diagnosis of iron deficiency anemia requires further investigation as to its cause. In adults, 60% of patients with iron deficiency anemia may have underlying gastrointestinal disorders leading to chronic fecal blood loss.[12] Other gastrointestinal causes include malaborption and celiac disease. Additional causes are dietary insufficiency, menstruation, diversion of iron to fetal erythropoiesis during pregnancy, intravascular hemolysis and hemoglobinuria or other forms of chronic blood loss should all be considered.
Treatment
Treating iron deficiency, even in the absence of anemia, can benefit patients with heart failure.[13]
If the cause is dietary iron deficiency, iron supplements, usually with iron (II) sulfate or iron amino acid chelate, can correct the anemia. Chelated iron is ten to fifteen times more bioavailable per mg and has none of the side effects of iron sulfate's sulfur content. If malabsorption is present, it may be necessary to administer iron parenterally (e.g., as iron dextran, which has largely been replaced by iron sucrose), as on the World Health Organization list of essential medicines, [14] Parenteral iron other than in chelated form, however, is generally poorly tolerated, and the earlier forms of chelated iron, such as iron dextran, were not without risk. The still-available dextran preparation carries a significant risk of anaphylactic shock,[15] and iron dextran, as opposed to iron sucrose, provided ferrous as well as the desired ferric iron ions.
The replacement dose of iron may be low.
- In the elderly, may be as little as 15 mg per day of elemental iron [16].
- In patients with inflammatory bowel disease, 106 mg/day may be adequate in most patients.[17]
Follow up evaluation with retesting of the hemoglobin (Hgb), hematocrit (Hct), and mean corpuscular volume (MCV) may help demonstrate whether the treatment has been effective. Testing of the reticulocyte count is another way to measure a response to iron therapy. Finally, ongoing testing of iron indices via the ferritin level and maybe total iron binding capacity (TIBC), and serum iron levels are imperative to avoid iron overloading.
Iron supplements must be kept out of the reach of children, as iron-containing supplements are a frequent cause of poisoning in the pediatric age group.
"Iron supplementation should be considered for women with unexplained fatigue who have ferritin levels below 50 μg/L". [18] In this trial, the average mean corpuscular volume was normal.
References
- ↑ Murray-Kolb LE, Beard JL (2007). "Iron treatment normalizes cognitive functioning in young women". Am. J. Clin. Nutr. 85 (3): 778–87. PMID 17344500. [e]
- ↑ Seward SJ, Safran C, Marton KI, Robinson SH (1990). "Does the mean corpuscular volume help physicians evaluate hospitalized patients with anemia?". J Gen Intern Med 5 (3): 187–91. PMID 2187961. [e]
- ↑ Kis AM, Carnes M (July 1998). "Detecting iron deficiency in anemic patients with concomitant medical problems". J Gen Intern Med 13 (7): 455–61. PMID 9686711. PMC 1496985. [e]
- ↑ Guyatt G, Patterson C, Ali M, Singer J, Levine M, Turpie I, Meyer R (1990). "Diagnosis of iron-deficiency anemia in the elderly.". Am J Med 88 (3): 205-9. PMID 2178409.
- ↑ Guyatt GH, Oxman AD, Ali M, Willan A, McIlroy W, Patterson C.Laboratory diagnosis of iron-deficiency anemia: an overview.J Gen Intern Med. 19927:145-53. Review. (Erratum in: J Gen Intern Med 1992;7:423) PMID: 1487761
- ↑ Thorpe SJ, Walker D, Arosio P, Heath A, Cook JD, Worwood M (1997). "International collaborative study to evaluate a recombinant L ferritin preparation as an International Standard.". Clin Chem 43 (9): 1582-7. PMID 9299937. [e]
- ↑ Thorpe SJ (2010). "The development and role of international biological reference materials in the diagnosis of anaemia.". Biologicals 38 (4): 449-58. DOI:10.1016/j.biologicals.2010.02.007. PMID 20338782. Research Blogging.
- ↑ Thomas C, Thomas L (2002). "Biochemical Markers and Hematologic Indices in the Diagnosis of Functional Iron Deficiency". Clin Chem 48 (7): 1066-76. PMID 12089176.
- ↑ Guyatt GH, Oxman AD, Ali M, Willan A, McIlroy W, Patterson C (1992). "Laboratory diagnosis of iron-deficiency anemia: an overview". J Gen Intern Med 7 (2): 145–53. PMID 1487761. [e]
- ↑ McGee S (August 2002). "Simplifying likelihood ratios". J Gen Intern Med 17 (8): 646–9. PMID 12213147. [e]
- ↑ 11.0 11.1 Savage D, Lindenbaum J (September 1986). "Anemia in alcoholics". Medicine (Baltimore) 65 (5): 322–38. PMID 3747828. [e]
- ↑ Rockey D, Cello J (1993). "Evaluation of the gastrointestinal tract in patients with iron-deficiency anemia". N Engl J Med 329 (23): 1691-5. PMID 8179652.
- ↑ Anker SD, Comin Colet J, Filippatos G, Willenheimer R, Dickstein K, Drexler H et al. (2009). "Ferric carboxymaltose in patients with heart failure and iron deficiency.". N Engl J Med 361 (25): 2436-48. DOI:10.1056/NEJMoa0908355. PMID 19920054. Research Blogging.
- ↑ Peter I Folb (18 October 2004), The Safety and Iron Dextran and a comparison wit Iron Sucrose for Intravenous Use: a Short Report to the World Health Organization Advisory Committee on the Safety of Medicines, World Health Organization
- ↑ Dexferrum (iron dextran injection) - Labeling Change, Food and Drug Administration, 16 October 2009
- ↑ Rimon E, Kagansky N, Kagansky M, Mechnick L, Mashiah T, Namir M, Levy S (2005). "Are we giving too much iron? Low-dose iron therapy is effective in octogenarians". Am J Med 118 (10): 1142-7. DOI:10.1016/j.amjmed.2005.01.065. PMID 16194646. Research Blogging.
- ↑ Gisbert JP, Bermejo F, Pajares R, Pérez-Calle JL, Rodríguez M, Algaba A et al. (2009). "Oral and intravenous iron treatment in inflammatory bowel disease: hematological response and quality of life improvement.". Inflamm Bowel Dis 15 (10): 1485-91. DOI:10.1002/ibd.20925. PMID 19408339. Research Blogging.
- ↑ Vaucher P, Druais PL, Waldvogel S, Favrat B (2012). "Effect of iron supplementation on fatigue in nonanemic menstruating women with low ferritin: a randomized controlled trial.". CMAJ 184 (11): 1247-54. DOI:10.1503/cmaj.110950. PMID 22777991. PMC PMC3414597. Research Blogging.
See Also
==External links==