Paracentesis: Difference between revisions
Jump to navigation
Jump to search

imported>Robert Badgett (New page: {{subpages}} A '''paracentesis''' is a medical "procedure in which fluid is withdrawn from a body cavity via a trocar and cannula, needle, or other hollow instrument."<ref>{{MeSH}}</ref><r...) |
Pat Palmer (talk | contribs) (resolving duplicate ref) |
||
| (10 intermediate revisions by 4 users not shown) | |||
| Line 1: | Line 1: | ||
{{subpages}} | {{subpages}} | ||
A '''paracentesis''' is a medical "procedure in which fluid is withdrawn from a body cavity via a trocar and cannula, needle, or other hollow instrument."<ref>{{MeSH}}</ref><ref name="pmid18334692">{{cite journal |author=Wong CL, Holroyd-Leduc J, Thorpe KE, Straus SE |title=Does this patient have bacterial peritonitis or portal hypertension? How do I perform a paracentesis and analyze the results? |journal=JAMA |volume=299 |issue=10 |pages=1166–78 |year=2008 |month=March |pmid=18334692 |doi=10.1001/jama.299.10.1166 |url=http://jama.ama-assn.org/cgi/pmidlookup?view=long&pmid=18334692 |issn=}}</ref> A paracentesis usually refers to removing [[ascites]]. | A '''paracentesis''' is a medical "procedure in which fluid is withdrawn from a body cavity via a trocar and cannula, needle, or other hollow instrument."<ref>{{MeSH}}</ref><ref name="pmid18334692">{{cite journal |author=Wong CL, Holroyd-Leduc J, Thorpe KE, Straus SE |title=Does this patient have bacterial [[peritonitis]] or [[portal hypertension]]? How do I perform a paracentesis and analyze the results? |journal=JAMA |volume=299 |issue=10 |pages=1166–78 |year=2008 |month=March |pmid=18334692 |doi=10.1001/jama.299.10.1166 |url=http://jama.ama-assn.org/cgi/pmidlookup?view=long&pmid=18334692 |issn=}}</ref><ref name="pmid17093242">{{cite journal |author=Thomsen TW, Shaffer RW, White B, Setnik GS |title=Videos in clinical medicine. Paracentesis |journal=N. Engl. J. Med. |volume=355 |issue=19 |pages=e21 |year=2006 |month=November |pmid=17093242 |doi=10.1056/NEJMvcm062234 |url=http://content.nejm.org/cgi/pmidlookup?view=short&pmid=17093242 |issn=}}</ref> A paracentesis usually refers to removing [[ascites]]. | ||
==Interpretation results== | ==Procedure== | ||
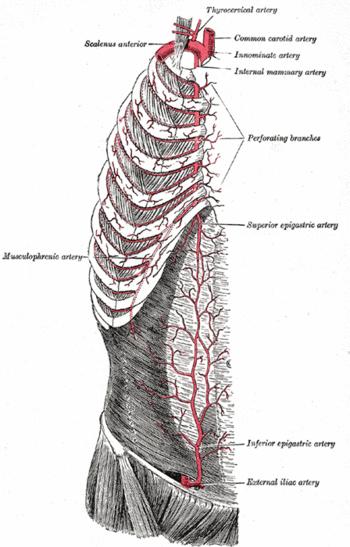
A serum-ascites albumin gradient (SAAG) of less than 1.1 g/dL lowers the probability of portal hypertension.<ref name="pmid18334692"/> | {{Image|Gray-image522.gif|right|350px|The location of the inferior epigastric artery within the sheath of the rectus muscle.}} | ||
Some experts recommend a over-the-needle catheter system.<ref name="pmid17093242">{{cite journal |author=Thomsen TW, Shaffer RW, White B, Setnik GS |title=Videos in clinical medicine. Paracentesis |journal=N. Engl. J. Med. |volume=355 |issue=19 |pages=e21 |year=2006 |month=November |pmid=17093242 |doi=10.1056/NEJMvcm062234 |url=http://content.nejm.org/cgi/pmidlookup?view=short&pmid=17093242 |issn=}}</ref> | |||
If a lower quadrant is used, inserting the needle lateral to the [[rectus muscle]] will avoid the [[inferior hypogastric artery]]. | |||
Routine [[ultrasonography]] can increase success rates according to a [[randomized controlled trial]].<ref name="pmid15915415">{{cite journal |author=Nazeer SR, Dewbre H, Miller AH |title=Ultrasound-assisted paracentesis performed by emergency physicians vs the traditional technique: a prospective, randomized study |journal=Am J Emerg Med |volume=23 |issue=3 |pages=363–7 |year=2005 |month=May |pmid=15915415 |doi= |url=http://linkinghub.elsevier.com/retrieve/pii/S0735675704003614 |issn=}}</ref> | |||
If more than 5 liters of ascites are removed, consider giving 6.25 g of albumin for each liter over 5 liters.<ref name="pmid3360270">{{cite journal |author=Ginès P, Titó L, Arroyo V, ''et al'' |title=Randomized comparative study of therapeutic paracentesis with and without intravenous albumin in cirrhosis |journal=Gastroenterology |volume=94 |issue=6 |pages=1493–502 |year=1988 |month=June |pmid=3360270 |doi= |url= |issn=}}</ref> | |||
==Interpretation of results== | |||
Cell count | |||
* Polymorphonuclear cells count of 250/mm<sup>3</sup> or more suggests [[spontaneous bacterial peritonitis]] | |||
Albumin | |||
* A serum-ascites albumin gradient (SAAG) of less than 1.1 g/dL lowers the probability of portal hypertension.<ref name="pmid18334692"/> | |||
Protein | |||
* Protein levels less than 1 g/dL have a high risk of [[spontaneous bacterial peritonitis]] during hospitalizations. | |||
Ph | |||
* "An ascitic fluid pH of lower than 7.35 ([[likelihood ratio]]=9.0) and a blood–ascitic fluid pH gradient of 0.10 or greater ([[likelihood ratio]]=11.3) were the most accurate thresholds for diagnosing [[spontaneous bacterial peritonitis]]" according to a [[systematic review]] by the [http://www.sgim.org/index.cfm?pageId=666 Rational Clinical Examination].<ref name="pmid18334692"/> | |||
Cultures | |||
==References== | ==References== | ||
<references/> | <references/> | ||
Revision as of 09:11, 30 August 2024
A paracentesis is a medical "procedure in which fluid is withdrawn from a body cavity via a trocar and cannula, needle, or other hollow instrument."[1][2][3] A paracentesis usually refers to removing ascites.
Procedure
Some experts recommend a over-the-needle catheter system.[3]
If a lower quadrant is used, inserting the needle lateral to the rectus muscle will avoid the inferior hypogastric artery.
Routine ultrasonography can increase success rates according to a randomized controlled trial.[4]
If more than 5 liters of ascites are removed, consider giving 6.25 g of albumin for each liter over 5 liters.[5]
Interpretation of results
Cell count
- Polymorphonuclear cells count of 250/mm3 or more suggests spontaneous bacterial peritonitis
Albumin
- A serum-ascites albumin gradient (SAAG) of less than 1.1 g/dL lowers the probability of portal hypertension.[2]
Protein
- Protein levels less than 1 g/dL have a high risk of spontaneous bacterial peritonitis during hospitalizations.
Ph
- "An ascitic fluid pH of lower than 7.35 (likelihood ratio=9.0) and a blood–ascitic fluid pH gradient of 0.10 or greater (likelihood ratio=11.3) were the most accurate thresholds for diagnosing spontaneous bacterial peritonitis" according to a systematic review by the Rational Clinical Examination.[2]
Cultures
References
- ↑ Anonymous (2024), Paracentesis (English). Medical Subject Headings. U.S. National Library of Medicine.
- ↑ 2.0 2.1 2.2 Wong CL, Holroyd-Leduc J, Thorpe KE, Straus SE (March 2008). "Does this patient have bacterial peritonitis or portal hypertension? How do I perform a paracentesis and analyze the results?". JAMA 299 (10): 1166–78. DOI:10.1001/jama.299.10.1166. PMID 18334692. Research Blogging.
- ↑ 3.0 3.1 Thomsen TW, Shaffer RW, White B, Setnik GS (November 2006). "Videos in clinical medicine. Paracentesis". N. Engl. J. Med. 355 (19): e21. DOI:10.1056/NEJMvcm062234. PMID 17093242. Research Blogging.
- ↑ Nazeer SR, Dewbre H, Miller AH (May 2005). "Ultrasound-assisted paracentesis performed by emergency physicians vs the traditional technique: a prospective, randomized study". Am J Emerg Med 23 (3): 363–7. PMID 15915415. [e]
- ↑ Ginès P, Titó L, Arroyo V, et al (June 1988). "Randomized comparative study of therapeutic paracentesis with and without intravenous albumin in cirrhosis". Gastroenterology 94 (6): 1493–502. PMID 3360270. [e]