Tuberculosis: Difference between revisions
imported>Nancy Sculerati |
imported>Nancy Sculerati No edit summary |
||
| Line 89: | Line 89: | ||
'''Latent TB''' is usually treated fairly easily with one to two medications, depending on local resistance patterns. The treatment often lasts up to a year. | '''Latent TB''' is usually treated fairly easily with one to two medications, depending on local resistance patterns. The treatment often lasts up to a year. | ||
===Inpatient and outpatient therapy: hospital or ambulatory care?=== | |||
===Compliance, noncompliance and resistant TB=== | ===Compliance, noncompliance and resistant TB=== | ||
'''Multi Drug Resistant TB (MDR-TB)''': Certain geographical areas have seen rises in "MDR-TB". This is especially a problem when patients are intermittently-compliant with their therapy, as the organism develops drug-resistance. | '''Multi Drug Resistant TB (MDR-TB)''': Certain geographical areas have seen rises in "MDR-TB". This is especially a problem when patients are intermittently-compliant with their therapy, as the organism develops drug-resistance. '''Active TB''' usually requires hospitalization and treatment with multiple medications. Given that the treatment regimen is lengthy and complicated, '''Directly Observed Therapy''' (DOT) is often recommended. There have been many legal and ethical issues involving involuntary isolation of non-compliant patients with active TB. | ||
====Directly Observed Therapy (DOT)==== | ====Directly Observed Therapy (DOT)==== | ||
Revision as of 15:35, 28 April 2007
Overview
Tuberculosis, also known as "TB" or "consumption", is a multi-system disease caused by a bacterial infection. Tuberculosis is always caused by the presence of the organism Mycobacterium tuberculosis in the tissues of the body. "The World Health Organization (WHO) estimates that 1722 million are infected with Mycobacterium tuberculosis." [1]
There are several other species of the genus Mycobacterium that are also human pathogens, but all of these organisms are of much lower virulence than Mycobacterium tuberculosis. That means that they are less apt to be able to invade the body and cause illness, and that even when they succeed in infecting a person, they cause less serious infection that is more often managed successfully by the body's own immune defenses. When such "minor" species of Mycobacteria cause disease in humans the illness is called Atypical tuberculosis, not tuberculosis.
This article is restricted to tuberculosis infection by Mycobacterium tuberculosis. Despite that narrow focus, the manifestations of human infection by this one organism are so variable that the article can only briefly discuss the more common presentations. Infections by M. tuberculosis range from a walled-off primary nidus of infection that causes no symptoms of disease (latent TB) to localized illness of the lungs, lymph nodes, or other body parts like the ears, voice box, that can range from mild to disabling, to a disseminated infection that is seeded throughout the entire body (Miliary TB) and is frequently fatal even with the most aggressive of available treatments.
As with organisms in any species, including bacteria, there are variations from one individual to the next. The tubercle bacillus is well known for individual strains that vary, independently, in both virulence and antibiotic resistance. In general, the severity of disease caused by TB infection is dependant on three major factors- the virulence (and dose) of the particular strain of TB a patient was exposed to, (2) the patients own physical integrity and immune competency (host resistance), and (3) timely treatment (or lack of timely treatment) with an appropriate selection of anti-tuberculosis drugs for a sufficiently prolonged period.
Epidemiology
Approximately one-third of the world population is infected with TB at any given time, with approximately 2 million TB-related deaths per year worldwide.
People with HIV disease, cancer, malnutrition, chemotherapy, drug or alcohol abuse are especially susceptible to developing active TB. TB rates and deaths are greatest in the developing world, and TB is one of the leading causes of death in people with HIV. In the United States, TB rates increased during the early years of the HIV epidemic, but have since declined, and are in fact the lowest they have been since surveillance began in 1953. However, TB still affects tens of thousands of Americans, and kills several hundred per year.
Globally, the highest rates of tuberculosis infection are in , and additional geographic regions with high endemic rates of infection include .
Infection in other species
Mycobacterium tuberculosis affects other vertebrates besides humans, and can be transmitted between species. One of the risks of non-pasteurized milk is drinking infected secretions from cows afflicted with bovine tuberculosis."Tuberculosis in cattle has been known even before classical times... Owing to its close resemblance with the disease in humans and the close relationships between the causative agents, they were initially termed M. tuberculosis typus bovinus and M. tuberculosis typus humanus."Michel AL. Implications of tuberculosis in African wildlife and livestock. [Review] [30 refs] [Journal Article. Review] Annals of the New York Academy of Sciences. 969:251-5, 2002 Oct. UI: 12381600
Elephants have been diagnosed with the disease, in captivity.(reference:Payeur JB. Jarnagin JL. Marquardt JG. Whipple DL. Mycobacterial isolations in captive elephants in the United States. Annals of the New York Academy of Sciences. 969:256-8, 2002 Oct. UI: 12381601)
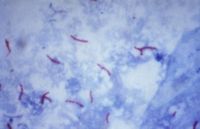
Microbiology
Natural History
Although it is possible to live with this infection for years, untreated, in the era "before effective drugs were available, 50% of patients with active pulmonary tuberculosis died within 2 years, and only 25% were cured." From: Chapter 248 - Mycobacterium tuberculosis TREATMENT OF TUBERCULOSIS in Mandell, Bennett, & Dolin: Principles and Practice of Infectious Diseases, 6th ed.
Tuberculosis can affect any organ in the body, but the primary disease is in the lungs. TB is usually spread by prolonged contact with someone with active pulmonary TB. This most often occurs in household contacts, or in people who work with an infected person in a workplace with poor ventilation.
Histopathology
When tuberculosis infects tissue the hallmark lesion is a granuloma.
Latent Tuberculosis
In most people, especially those who have a normal immune system, after becoming infected, the body controls the illness. They have no symptoms, and are not contagious. Signs of infection can be a positive TB test or typical changes on X-rays of the chest. In a small, but significant, percentage of people, latent TB can "reactivate" and make the person ill. Therefore, most people with latent TB are treated to eliminate the infection.
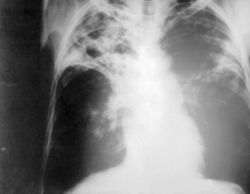
Active Pulmonary Tuberculosis
In some people, the initial infection can make them ill, in others, latent TB reactivates and makes them ill. In pulmonary tuberculosis the usual symptoms are cough for longer than three weeks, bloody sputum, fevers, night sweats, and weight loss. At this stage, the disease is very contagious, and is likely to eventually be fatal if not treated.
Extrapulmonary Tuberculosis
Gastrointestinal tuberculosis
When people with pulmonary tuberculosis are not treated with an effective combination of antibiotics, the bacteria multiply and are present, in great and ever increasing quantity, in the secretions coughed up from the lungs. This sputum touches the lining of the mouth, the back of the nose, and is also swallowed, and, unless treatment to stop the multiplication of the bacteria is instituted, lodges in the stomach and intestines of patients with pulmonary TB. Even though stomach acid has some killing effect on the bacteria, if the numbers are large enough, there are survivors that exit the anus. At any point along the uper airway tract and gastrointestinal tract, adherence of the bacteria may lead to an infection, with the formation of a non-healing ulcer.
About 70% of individuals with advanced stages of pulmonary tuberculosis have active infections in their GI tract seeded through swallowing secretions coughed up from the lungs, and so have both pulmonary TB and a form of extrapulmonary TB that was contracted secondary to their pulmonary infection.
Laryngeal Tuberculosis
Pott's Disease
Tuberculosis Adenitis ("Scrofula")
Disseminated Tuberculosis (Miliary TB)
Making the diagnosis
Treatment
"A fundamental problem in the treatment of tuberculosis (TB) is the long duration of therapy required for cure." (quote:Why Is Long-Term Therapy Required to Cure Tuberculosis? Connolly LE, Edelstein PH, Ramakrishnan L PLoS Medicine Vol. 4, No. 3, e120 doi:10.1371/journal.pmed.0040120). Although anti-bacterial drugs given to treat other infections are rarely if ever called "chemotherapy", that term is ordinarily appled to the courses of antibiotics used for the treatment of Mycobacterium tuberculosis. Despite the use of the word, none of these medications are similar to the anti-cancer drugs that are the agents most often meant by the term.
In all bacteria infections, antibiotic treatment affects the bacteria when they are actively reproducing. That means that bacteria like M. tuberculosis are not quick to be killed even by antibiotics that are capable of killing them, because the bacteria can become dormant and reproduce very slowly. Additionally, the tubercle bacillus can be protected by the tissue damage that it causes. In other words, when tuburculosis causes pulmonary tissue and lymph nodes to become necrotic, the blood supply to these tissues is compromised and even if the patient is taking an adequate dose of a set of antibiotics that will kill replicating bacteria, those bacteria in the tissues that do not receive a normal blood supply will not be exposed to the antibiotics in the blood.
Additionally, the patient's immune system is also designed to kill the bacteria when they are dividing and is less able to eradicate a dormant infection than the same number of bacteria that are actively dividing. Further, the necrotic and cavitary tissue sequesters the bacteria from the circulating cells and antibodies of the immune system, and protects the bacteria from the patient's host defenses.
If the bacteria are exposed to antibiotics that do not wipe them out, then resistant organisms may multiply and, through genetic factors, drug resistant strains can become the predominant ones in the infection.
Drugs against TB: Antituberculous chemotherapy for treatment, Antituberculous prophylaxis for prevention
The first efficacious drugs to treat TB became available in different arts of the wrld in the 1940's and 1950's, before that time - treatment consisted on long-term hospitalization that focused both on quarrentining the patient from society and on increasing host resistance.
Isoniazid
Rifampin
Pyrazinamide
Ethambutol
Streptomycin
Fluoroquinolones
Latent TB is usually treated fairly easily with one to two medications, depending on local resistance patterns. The treatment often lasts up to a year.
Inpatient and outpatient therapy: hospital or ambulatory care?
Compliance, noncompliance and resistant TB
Multi Drug Resistant TB (MDR-TB): Certain geographical areas have seen rises in "MDR-TB". This is especially a problem when patients are intermittently-compliant with their therapy, as the organism develops drug-resistance. Active TB usually requires hospitalization and treatment with multiple medications. Given that the treatment regimen is lengthy and complicated, Directly Observed Therapy (DOT) is often recommended. There have been many legal and ethical issues involving involuntary isolation of non-compliant patients with active TB.
Directly Observed Therapy (DOT)
Increasing host resistance
The sanatoriums that served as treatment centers for tuberculosis patients in the pre-antibiotic era helped reduce the spread of infection by effecting a partial quarentine, but also served to increase patient's resistant to the progression of disease by XXX.
Nutrition
Reduction of bacterial load
Decreased host resistance
Immunosuppression
AIDS (HIV)
Organ transplant recipients
Infection control
Public health
In hospital
Reducing the rate of resistant TB
References
- ↑ Watters DA. Surgery for tuberculosis before and after human immunodeficiency virus infection: a tropical perspective. British Journal of Surgery. 84(1):8-14, 1997 page 8.
- http://www.cdc.gov
- Mandell, Douglas and Bennett's Principles and Practice of Infectious Diseases, Chirchill Livingstone.